Back Pain or Something More? When Does a Spine Tumor Require Surgery?
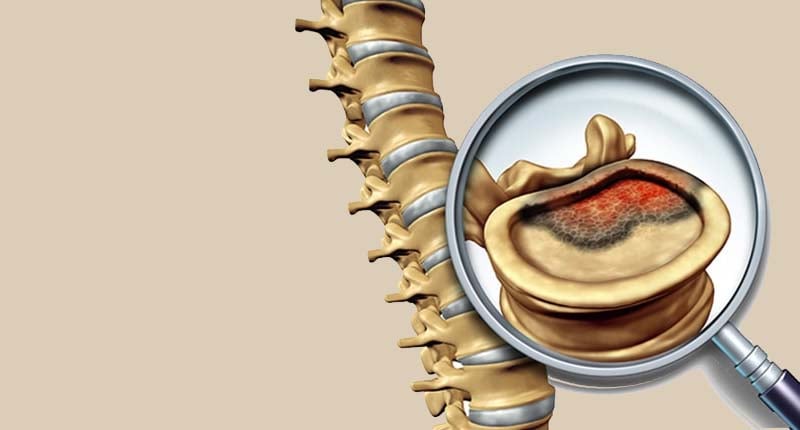
When a diagnosis involves the spine, the first question is almost always: 'Will I still be able to walk?' In 2026, spine tumor care has shifted from 'aggressive removal' to 'functional preservation.' Surgery is no longer the default; it is a precision tool used specifically to protect your mobility and rebuild the structural integrity of your back
Many spine tumors never need surgery and can be managed safely with observation or targeted radiation. Surgery becomes necessary only when the tumor threatens the strength of the spine or begins to press on the delicate nerves of the spinal cord.
Understanding when surgery is truly needed helps replace fear with clarity. Spine tumor surgery today is not about being aggressive. It is about stepping in at the right moment to prevent permanent nerve damage and preserve movement.
What Are Spine Tumors?
Spine tumors are abnormal growths that occur in or around the spinal column. These tumors may arise from the bones of the spine, the spinal cord, or the tissues surrounding the nerves.
- Some spine tumors are benign, meaning they do not spread to other parts of the body. Others are malignant, either starting in the spine or spreading there from another cancer elsewhere. The behavior of the tumor often matters more than its name.
- Doctors also distinguish between primary spine tumors, which begin in the spine itself, and metastatic spine tumors, which spread from organs such as the lung, breast, or prostate. Metastatic tumors are more common and often affect the strength of the spinal bones.
Location plays a critical role in decision-making. A small tumor pressing on the spinal cord may cause serious symptoms, while a larger tumor in a stable area may cause none. This is why treatment decisions focus on nerve involvement and spinal stability, not size alone.
Do All Spine Tumors Require Surgery?
No. Many spine tumors never require surgery. Doctors always look for the safest option that protects movement and quality of life.
Some tumors grow very slowly and cause no pressure on the spinal cord or nerves. In these cases, doctors may recommend regular imaging and observation. Careful monitoring allows treatment only if the tumor changes or symptoms appear.
Other spine tumors respond well to radiation therapy or targeted treatments. When a tumor shrinks or stabilizes with non-surgical care, and the spine remains strong, surgery offers no added benefit.
Doctors avoid spine surgery unless there is a clear reason. Surgery carries risks, so it becomes an option only when the danger of not operating outweighs the risks of the procedure.
When Do Doctors Recommend Surgery for Spine Tumors?
Doctors recommend surgery when a spine tumor begins to threaten nerve function or the structural strength of the spine. At this point, surgery shifts from optional to necessary.
- Progressive Neurological Symptoms: Weakness, numbness, or difficulty walking signal nerve compression. These symptoms often worsen if untreated. Surgery helps relieve pressure before permanent damage occurs.
- Spinal Cord or Nerve Compression: Tumors pressing on the spinal cord or nerve roots can cause pain, loss of sensation, or coordination problems. Surgical decompression protects nerve signals and function.
- Loss of Spinal Stability: Some tumors weaken the spinal bones. This weakness increases the risk of fractures or collapse. Surgery stabilizes the spine using modern fixation techniques.
- Failure of Non-Surgical Treatments: When radiation or medication fails to control symptoms, surgery becomes necessary. Persistent pain or worsening function often drives this decision.
In these situations, surgery serves a protective role. The goal is not just tumor removal, but preserving movement, balance, and independence.
How Do Neurological Symptoms Influence the Decision for Surgery?
Neurological symptoms often provide the clearest signal that surgery may be necessary. These symptoms tell doctors that the tumor is no longer just present; it is interfering with nerve function.
- Weakness or Loss of Strength: Difficulty lifting a foot, gripping objects, or standing steadily often points to nerve compression. When weakness progresses, waiting can increase the risk of permanent damage.
- Numbness or Tingling: Persistent numbness, pins-and-needles sensations, or altered feeling in the arms or legs suggest pressure on nerve pathways. Surgery may be needed to prevent further sensory loss.
- Balance and Coordination Problems: Unsteadiness or frequent falls can happen when the cord becomes compressed. These changes affect safety and independence. Early surgical relief can prevent long-term disability.
- Changes in Bladder or Bowel Control: Loss of bladder or bowel control represents a serious warning sign. Doctors treat this as a priority situation. Surgery is often urgent to preserve remaining nerve function.
Neurological symptoms help doctors judge timing. The goal is not to wait until damage becomes permanent, but to intervene while recovery remains possible.
When Is Surgery Needed to Relieve Spinal Cord Compression?
Spinal cord compression develops when a tumor presses directly on the spinal cord or nearby nerve roots. This situation requires careful and often timely surgical decision-making.
- Pressure on the Spinal Cord: Even a small amount of pressure can disrupt nerve signals. Surgery removes or reduces this pressure to protect movement and sensation.
- Rapid Symptom Progression: Symptoms that worsen over days or weeks raise concern. Fast progression suggests active compression. Surgery helps stop further neurological decline.
- Risk of Permanent Nerve Damage: Prolonged compression can lead to irreversible weakness or paralysis. Doctors act before this threshold is crossed.
- Emergency vs Urgent Surgery: Some cases require immediate surgery, especially when walking or bladder control is affected. Others allow short-term planning but still need timely intervention.
In these situations, surgery acts as a rescue measure. The aim is not only tumor control but also the preservation of the ability to move, feel, and function.
The Shift to Keyhole Procedures
The 'big scar' spine surgeries of the past are being replaced by Minimally Invasive Spine Surgery (MISS). Using specialized tubes and microscopic cameras, surgeons can now treat tumors through incisions as small as a postage stamp. For patients, this means the 'long-term disability' they feared is replaced by a recovery that often sees them back on their feet in just a few days.
How Does Spinal Instability Affect the Need for Surgery?
Spinal instability means the spine can no longer support the body safely. When a tumor weakens the spine's bones, surgery is often necessary to prevent collapse and preserve movement.
- Bone Weakening Caused by the Tumor: Some spine tumors eat away at the vertebrae. As the bone weakens, even everyday activities like standing or walking can become risky.
- Risk of Fracture or Vertebral Collapse: A weakened vertebra may suddenly crack or collapse. It can cause severe pain and sudden nerve injury. Surgery helps prevent these events before they happen.
- Pain That Increases With Movement: Pain that advances when standing, sitting, or turning often points to instability. This type of pain differs from nerve pain and signals a structural problem.
- Need for Surgical Stabilization: Surgeons may use rods, screws, or bone cement to restore strength. The goal is to rebuild stability so the spine can safely carry weight again.
In these cases, surgery does not focus only on the tumor. It focuses on rebuilding the spine so patients can move without fear of collapse.
When Can Spine Tumors Be Managed Without Surgery?
Many spine tumors can be treated safely without surgery. Doctors choose non-surgical care when the tumor does not threaten nerves or spinal stability.
- Small or Slow-Growing Tumors: Some tumors grow very slowly and cause no symptoms. Regular imaging allows doctors to monitor changes over time. Treatment begins only if the tumor progresses.
- No Neurological Symptoms: Patients without weakness, numbness, or balance problems often avoid surgery. Preserved nerve function lowers urgency. Observation remains safe in these cases.
- Stable Spinal Structure: When the spine remains strong and aligned, surgery offers no structural benefit. Stability allows non-invasive treatments to work effectively.
- Tumors Responsive to Radiation or Medication: Certain tumors respond well to radiation therapy or systemic treatments. Shrinkage or control without surgery reduces risk. Doctors monitor the response closely.
- Patients With High Surgical Risk: Some patients cannot tolerate surgery due to other health conditions. Non-surgical care offers safer alternatives for symptom management.
Radiation isn't just 'backup' anymore. Technologies like CyberKnife allow us to deliver high-dose radiation to a spine tumor with sub-millimeter precision, often avoiding surgery entirely for tumors that aren't causing structural instability. However, if the tumor has already caused the bone to collapse, radiation cannot fix the 'architecture,' and that is where the surgeon's skill becomes irreplaceable.
How Do Doctors Decide Between Surgery and Radiation for Spine Tumors?
Doctors compare surgery and radiation based on what each treatment can realistically achieve. The decision focuses on function, safety, and long-term outcome.
- Purpose of Each Treatment: Surgery relieves pressure, stabilizes the spine, and protects nerves. Radiation controls tumor growth. Each serves a different role.
- Tumor Sensitivity to Radiation: Some tumors respond strongly to focused radiation. Techniques like stereotactic radiotherapy can control these tumors without incisions.
- Structural Condition of the Spine: Radiation cannot repair weakened or collapsed bones. When instability is present, surgery is necessary before or instead of radiation.
- Speed of Symptom Progression: Rapid neurological decline often favors surgery. Radiation works over time and may not act fast enough in urgent situations.
- Multidisciplinary Evaluation: Specialists review imaging together before making a decision. This collaboration balances risks and benefits. Combined approaches often deliver the best results.
In many cases, surgery and radiation work together. Stabilization and decompression come first, followed by radiation for tumor control.
What Are the Goals of Spine Tumor Surgery?
Spine tumor surgery focuses on protecting function, not just removing tissue. Surgeons plan every step with long-term mobility and safety in mind.
- Relieve Pressure on Nerves and the Spinal Cord: Removing compression helps restore nerve signals. Early relief improves the chance of regaining strength and sensation.
- Stabilize the Spine: Tumors can weaken the bones that support the body. Surgery rebuilds strength using modern fixation techniques. Stability allows safe movement again.
- Reduce Pain: Pain often improves when pressure and instability are corrected. Many patients notice meaningful relief after recovery begins.
- Preserve or Restore Mobility: The main goal is to keep patients walking and independent. Surgical planning prioritizes movement and balance.
- Create a Safe Path for Additional Treatment: Surgery may prepare the spine for radiation or systemic therapy. Stabilization allows other treatments to work safely.
Spine tumor surgery aims to protect the quality of life. Success focuses on function as much as tumor control.
What Risks Do Doctors Consider Before Recommending Spine Surgery?
Doctors weigh the benefits of surgery against potential risks very carefully. Surgery becomes an option only when the benefits clearly outweigh the concerns.
- Neurological Risk: Operating near the spinal cord and nerves carries risk. Surgeons use advanced planning to minimize injury. Protecting nerve function remains the top priority.
- Bleeding and Infection: Spine surgery involves blood vessels and deep tissue. Care teams follow strict safety protocols to reduce complications.
- Recovery and Rehabilitation Needs: Recovery varies based on surgery type and patient health. Some patients need physiotherapy to regain strength and confidence.
- Overall Health and Medical Fitness: Doctors assess heart, lung, and general health before surgery. Medical readiness influences timing and approach.
- Use of Intraoperative Monitoring: Modern surgery uses real-time nerve monitoring. This technology helps surgeons detect nerve stress in real time. Monitoring adds an important layer of safety.
Conclusion
At the end of the day, deciding on spine surgery isn't just a medical choice. It is a choice to protect your future self. If you have noticed that your back pain keeps you up at night, or if you feel a sudden, strange unsteadiness in your step, your body is simply telling you it needs a little extra support.
We never view surgery as the first or only answer. Instead, we see it as a way to reinforce your foundation so you can keep living your life on your own terms. At Qonaq, we focus on bringing you together with specialists who treat you like a person, not a patient.
By using tools like intraoperative nerve monitoring, which act as a high-tech guardian of your safety during a procedure, we ensure that every step in the operating room is focused on protecting your nerves. Your ability to move is your freedom, and keeping you moving safely is our highest priority.
Related Hospitals
Discover hospitals and medical centers related to this topic for quality healthcare services.

MGM Healthcare, Chennai
MGM Healthcare, Chennai, is a 400-bed quaternary-care super-specialty hospital accredited by JCI, NABH, and NABL. The hospital features 100 ICU beds, ...
Accreditations


Facilities

Paras Hospital, Gurgaon
Paras Hospital, Gurgaon, established in 2006, is a 300-bed NABH- and NABL-accredited tertiary care hospital offering over 36 super specialties. The ho...
Accreditations

Facilities

Medanta - The Medicity Hospital, Gurgaon
Medanta – The Medicity in Gurgaon is one of India's largest and most advanced multi-speciality hospitals, founded in 2009 by world-renowned cardiac su...
Accreditations


Facilities

BLK-Max Super Speciality Hospital, New Delhi
BLK-Max Super Speciality Hospital in New Delhi is one of India's premier healthcare institutions, offering 650 beds, 22 advanced operation theatres, a...
Accreditations


Facilities

Max Super Speciality Hospital, Saket, Delhi
Max Super Speciality Hospital, Saket, New Delhi, is a leading JCI- and NABH-accredited hospital offering advanced medical care across 38+ specialities...
Accreditations



Facilities

Fortis Memorial Research Institute (FMRI), Gurgaon
Fortis Memorial Research Institute (FMRI), Gurgaon, is a world-class multi-specialty hospital established in 2013. The hospital offers 330 beds, 15 op...
Accreditations


Facilities
Related Doctors
Connect with experienced doctors and medical specialists in this field.

Dr. Deshpande V Rajakumar
Director

Dr. Ashok Kumar Singhal
Senior Consultant

Dr. Agnivesh Tikoo
Senior Consultant

Dr. Shishir Shetty
Head of Department (HOD)

Dr Shekhar G Patil
Senior Consultant

Dr. Nirmala S
Senior Consultant
Related Articles
Explore more articles and insights on similar health topics.

How Long Can You Live After an Organ Transplant?
Who Can Get an Organ Transplant in India? Eligibility Rules Explained
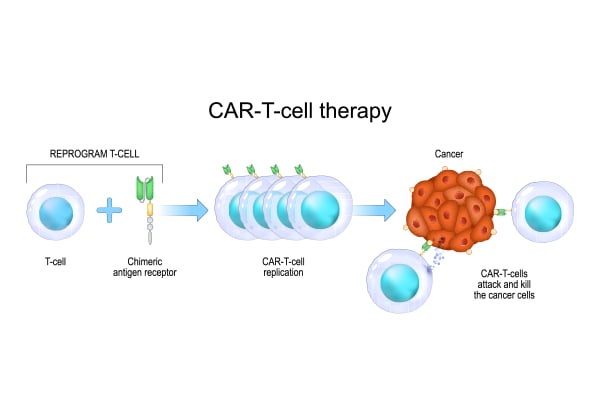
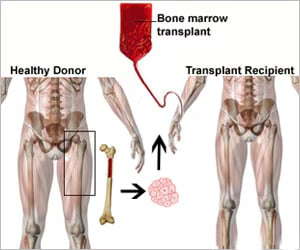
Bone Marrow Transplant vs CAR-T Cell Therapy: Which Is Better for Blood Cancer?
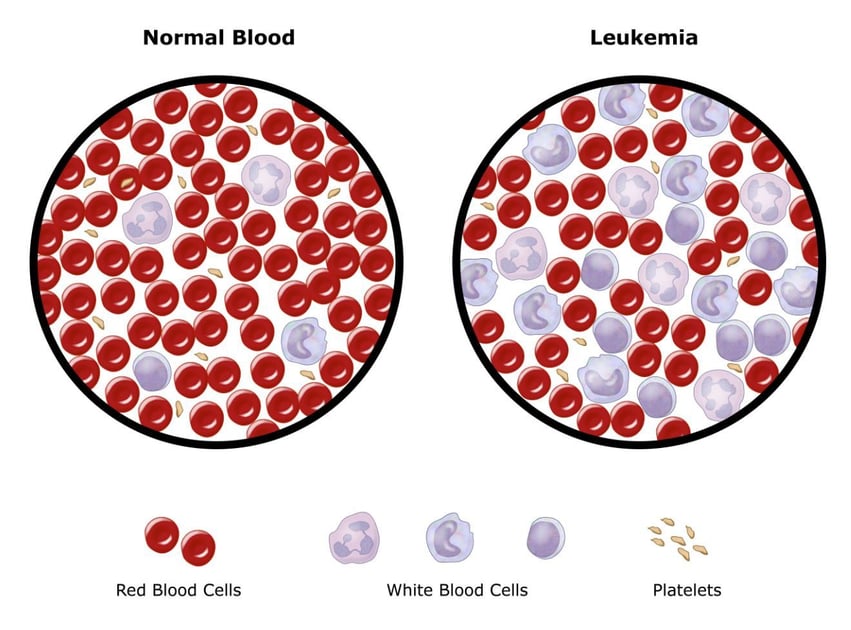
Can You Survive Leukemia Without a Bone Marrow Transplant?
Is Bone Marrow Transplant Worth the Cost? A Financial and Medical Guide for International Patients in India
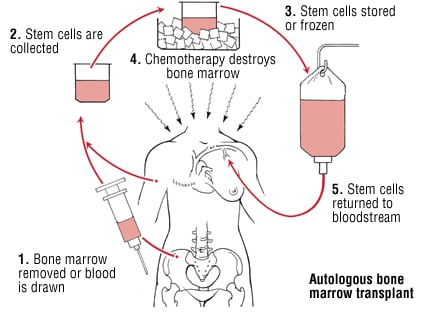
Is Bone Marrow Transplant Safe for International Patients?
Author
View AllDr. Deepanshu Siwach is an experienced clinical pharmacist with a Doctor of Pharmacy degree. He has over 4 years of experience and has worked with thousands of patients. He has been associated with ... Read More
Our website uses cookies. By clicking on accept you give your consent to the use of cookies as per our Privacy Policy.

